Services
FILLINGS
When a tooth structure has been lost due to caries or trauma, a filling can then be placed to restore normal anatomy and to seal the site from future decay. Several different filling materials are available, each with specific pros and cons which are considered carefully based on the site and size of the cavity as well as other relevant factors.
AMALGAM FILLINGS
Amalgam refers to the metal fillings that have been used in the United States since 1833. Amalgam means “mixture”, and in this case refers to a mixture of mercury, silver, tin, copper. It has good strength if placed with enough thickness, and has good longterm durability. It is not sensitive to fluid, and may be placed even in areas where isolation from blood or saliva cannot be achieved. Unfortunately, to achieve proper thickness such that it will not fracture, a deep enough cavity must be prepared in the tooth, often much deeper and closer to the nerve than the removal of decay alone would require. Because amalgam has no bonding properties, the cavity must then be shaped wider at the base than at the top in order to hold the filling in mechanically. This requires removal of even more tooth structure. The popularity of amalgam has decreased in recent years due to environmental concerns (mercury disposal), popular health concerns (due to mercury content), esthetic concerns, and the availability of newer materials with improved characteristics, safety, reliability and esthetics. While several European countries have banned the use of amalgam, its use is still permitted in the United States, with strict environmental controls imposed on dentists.
COMPOSITE FILLINGS
Composites are made of resin with silica (glass) filler which provides wear resistance. Unlike amalgam, composite materials are bonded to the enamel and dentin of the tooth; therefore, they do not require a specific shape or size of the cavity preparation. This conserves tooth structure and protects the nerve. Because composite bonds to the walls of the tooth, the tooth and filling move as one cohesive unit during chewing. This prevents flexure of the tooth walls around the filling and ultimate fracture of the tooth, a common problem often seen with aging amalgam fillings.
INLAY & ONLAY RESTORATIONS
Inlays and onlays are fillings made of gold or porcelain which are bonded onto the tooth to restore its anatomy after tooth fracture or removal of significant amount of decayed tooth structure. Due to increased wear resistance and strength, these restorations last longer and can be used to replace larger areas of tooth than amalgam or composite.
CROWNS
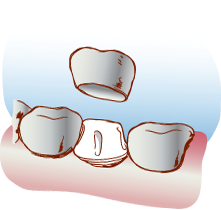
A crown is necessary when a tooth has fractured or when enough tooth structure is missing that the tooth requires full coverage to maintain its strength and function. Crowns are made from a wide range of different materials, each chosen for a specific characteristic which would meet the clinical situation. Choosing the correct material requires a dentist’s expertise and experience; however, a patient’s input is often important where esthetics are concerned. Good communication is important and encouraged between doctor and patient to best select a material that meets all clinical, functional and esthetic requirements.
VENEERS
A veneer is a thin layer of porcelain or similar material which is bonded to the fronts of existing teeth to change the shape, size and/or color. Veneers can make short teeth longer, long teeth shorter, crooked teeth appear straight, improve the smile line, close gaps, improve shape and cover white spots and other discolorations. Veneer cases require planning and good communication to achieve spectacular results. As such, several consult appointments are usually best to ensure that what the patient desires is achievable and well-understood by the dentist. Impressions and photographs are taken at the first consult. After the models are ready and the case has been mounted and studied, the dentist will then revisit with the patient to show mock-up models and before/after photos. Patients often get a clearer idea of what they want when they can see the possibilities. Final tooth color, size, shape and position can then be selected. After the plan is finalized, the patient is scheduled for the prepping of the teeth (if necessary) and the final impression is made and sent to the dental laboratory. Temporary restorations which mimic the final veneers will be cemented into place. When the veneers are ready, the patient returns for final try-in and cementation of his/her new smile.
ENDODONTICS (ROOT CANALS)
We find that this most dreaded of procedures is usually pretty anti-climatic. So try not to get too worried about it ahead of time. Only a very small percentage of root canal procedures are painful; mostly they are just long and boring for the patient because they are so technique sensitive for the dentist. A root canal consists of the removal of the inflamed or dead nerves from inside the roots of the tooth, disinfection of the empty canals, and filling/sealing of the clean canals. If a tooth is very infected, sometimes medication will be placed inside the tooth with a temporary filling and a second visit scheduled to fill and seal. During the procedure, the tooth is numbed, and the patient is given the option to use a mouth prop for better comfort. In our office, we do most of our patients’ root canals. We use a state-of-the-art rotary system and warm fill technology to achieve optimum shape and disinfection of canals and the tightest seal and most homogenous fill possible. There are situations, however, when we will refer a patient to an endodontist. This decision is made based on the tooth anatomy, diagnosed obstruction of the canals, or unclear symptoms. Most modern endodontists perform root canals under microscopy which improves their ability to navigate more difficult anatomy/structural defects. We are happy to share our patients with these skilled practitioners when we feel that their advanced skills are required for the best outcome for our patients.
IMPLANTS
When a tooth is missing and the patient is motivated to replace it, an implant is an ideal treatment, provided there is appropriate amount of healthy bone in which to place it. The implant itself is a screw-like cylindrical construct made out of titanium, ceramic or both which serves as the replacement of the tooth root. Once the bone has integrated with the implant surface, the implant is ready to be restored. An abutment is secured into the internal screw inside the implant and sits above the gumline as if it were a tooth that had been shaped for a crown. Then impressions are taken and a crown is fabricated and cemented onto the abutment. When this process is completed, the patient has a “tooth” which is not only functional, but is also not susceptible to decay.
Implants can also be used to support multi-unit bridges and to “snap” down dentures.
The critical step to the success of implant therapy is treatment planning. Implants should never be placed at the convenience of a surgeon who has been given no restorative guidance. It is critical that the implant surgeon/periodontist and the restorative dentist communicate seamlessly from start to finish to ensure proper fit and beautiful esthetics. A restorative dentist must first take impressions, create study models and fabricate a surgical guide. The surgeon then uses the guide during surgery to properly angulate and position the implant in the bone such that when the abutment and crown are prepared, the fit is the same as -or even better than – the original tooth.
We are proud to work as a team with a handful of carefully selected local surgeons and periodontists whose focused communication and excellent skills yield predictable outcomes for our patients time and time again.
DENTURES
As the saying goes, “dentures are a substitute for no teeth, not a substitute for teeth”. This is because “false teeth” function completely differently than do real teeth. As such, it takes a true understanding of edentulous (toothless) anatomy and function to properly fabricate dentures that fit properly, function properly and look natural. This process takes time; opportunities for try-ins to assess fit, speech, and esthetics prior to final processing are critical to the final result. Anyone can make dentures in an hour, but few would want to wear them. Dr. Cochrane has had advanced training in prosthodontics and is comfortable with the extra steps that it takes to make a well-fitting denture.
From the Front Desk
How are you sleeping? Your dentist wants to know
By Katie Dastoli, RDH If a survey was conducted in a room full of adults asking them how they are sleeping, it is likely that the majority would respond, “not …Read More »

